Learn more about how RashoRx Precision LLC revolutionizes precision medicine
Need a detailed pharmacogenomics test?


Pharmacogenomics is a branch of medicine that looks at how your genes can affect how you respond to medications. Also known as PGx testing, it can help tailor the most effective medications and dosages for the patients. At the same time, it helps identify and reduce the risk of side effects and increases the effectiveness of your treatment.

Pharmacogenomics is a branch of medicine that looks at how your genes can affect how you respond to medications. Also known as PGx testing, it can help tailor the most effective medications and dosages for the patients. At the same time, it helps identify and reduce the risk of side effects and increases the effectiveness of your treatment.
We offer comprehensive pharmacogenomics tests and consultation services to help you make the most informed decisions about your healthcare profile. By understanding how your genetics interact with different medications, you can ensure you take the most effective drugs and dosages for your body. Our pharmacogenomics testing assesses and analyzes clinically important genetic variations in your DNA to identify and predict how you respond to different medications.
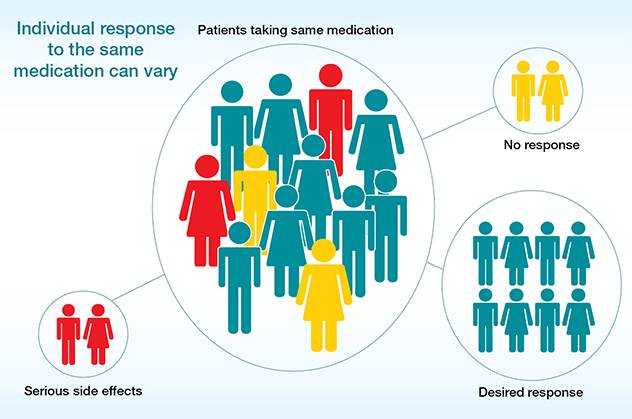
Everyone has unique genes that code for enzymes that are needed to activate or break down a medication. The level of activity of an enzyme (slow, intermediate, fast acting) will determine how the body will react to that medication. There are many people who are on clopidogrel (Plavix), an inactive drug, which requires the enzyme CYP2C19 to activate before it can have its therapeutic effect.
If a patient is a poor metabolizer of CYP2C19, the enzyme is not able to activate clopidogrel; therefore, the concentration of active metabolite is greatly decreased to almost none. This can cause therapeutic failure and put patients at risk for stroke or heart attacks. A pharmacogenomics test before a patient starts clopidogrel could be a life changer for a patient. It can be a life-and-death situation in some cases. So, pharmacogenomics plays a key factor in many disease states.
There are many people who are on omeprazole (Prilosec) for stomach acid, which is a CYP2C19 inhibitor. This is the same enzyme needed for activation of clopidogrel. Taking both would inhibit the activation of clopidogrel, which again means no therapeutic effect. This is a classic example of a drug-gene interaction.
With a painless cheek swab, a pharmacogenomics test can be done to help understand genetic makeup so that medications can be personalized. Learn more
According to the World Health Organization (WHO), major depressive disorder will be a major cause of disability by 2030. The current prescribing model is based mainly on trial and error. It can take months for a patient to get to a therapeutic level. The pharmacogenomic testing for antidepressant treatment can be used as a tool to guide therapy, which can cut down the time to get to the therapeutic level and get to the right medication right from the start.
The drug-gene test (PGx) can also be used in guiding cancer treatment where drug resistance and severe side effects are the major barriers. Genetic variance in some patients can interfere with their ability to process their medications. For example, the chemotherapy can put a patient at risk. The FDA requires pharmacogenomics testing on some medications ahead of starting chemotherapy.

The current practice model for prescribing medications related to mental health is a lengthy trial-and-error process. We have counseled numerous patients on managing their chronic conditions and have seen them go through 6 to 9 months of mental instability before they find the medication that works for them. We wanted to change that and shorten the time it takes to achieve the quality of life they deserve.
Every medication works differently for every single one of us. There are many factors that play a part in how the body reacts to a medication, including age, race, sex, and genetic makeup. Pharmacogenomics testing has been around for a very long time, but many providers do not have the time to implement that in their daily practice. More importantly, there is a huge gap in being able to interpret the complex raw data into an actionable clinical plan. So, we wanted to change that.
Utilizing a trained pharmacogenomics-certified pharmacist as part of an interdisciplinary team can give providers and their patients the power to increase the quality of care. The extensive training our pharmacists go through fills in the huge gap by creating a one-page summary of an actionable plan. This is called precision medicine, where medications are personalized based on a patient’s genetic makeup.
Crack the code for which medication works for a patient and Improve patient outcomes. Billions of prescriptions are filled every year. However, therapeutic response rates for many drugs are only 50-75%. Because of that, providers often are stuck using trial and error to find a medication and a dose that works well for their patients, negatively impacting patient outcomes and satisfaction. Pharmacogenomics testing and pharmacist insight can help optimize medication selection based on genetic makeup and reduce time, avoid trial and error, and negative outcomes.
The process includes 4 simple steps:
Let’s start the journey towards success and enhance revenue for your business. Take your company to the next level.



Pharmacogenomic testing is beneficial for both healthcare providers and patients. Here are some important benefits of PGx testing.
Patients can experience substantial healthcare benefits with PGx testing. Check out the key advantages of PGx testing for patients.
Don’t miss our future updates! Get Subscribed Today!
Copyright © 2024 Rasho Rx Precision LLC | Powered by Rasho Rx Precision LLC